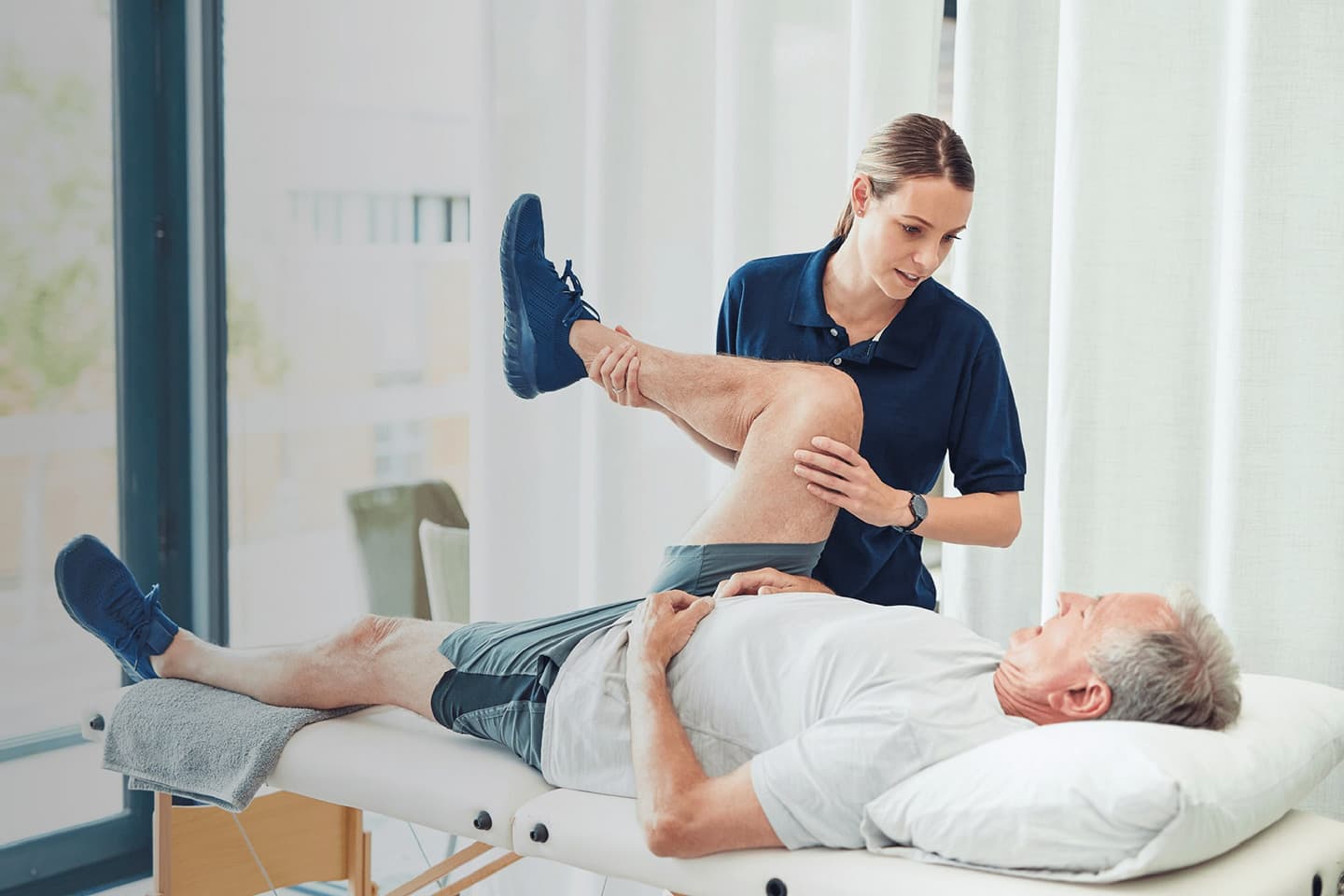
Physical therapy is a healthcare specialty focused on helping individuals improve their movement and manage pain through physical interventions. Physical therapists (PTs) assess, diagnose, and treat a wide range of conditions, from musculoskeletal injuries and neurological disorders to post-surgery recovery and chronic pain management. They use techniques such as exercise, manual therapy, heat and cold treatments, and electrical stimulation to enhance mobility, strength, and function.
Physical therapy aims to restore independence, reduce pain, and improve overall quality of life by addressing the physical impairments that limit a patient’s ability to perform daily activities.

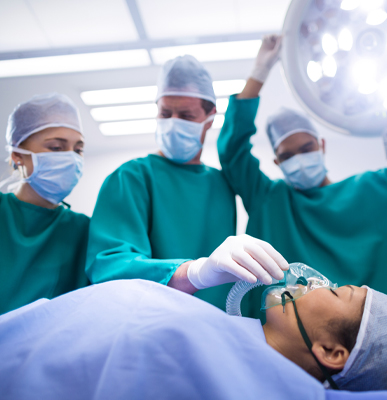

Physical therapy has several specialized branches, each focusing on different aspects of rehabilitation and patient care. These include:
These branches ensure that physical therapy addresses a wide range of health conditions, providing specialized care to improve mobility, function, and quality of life for patients across all ages and backgrounds.
Nerve Conditions in Physical Therapy: Their Treatment and Prevention
Nerve conditions in physical therapy refer to disorders that affect the nerves and can lead to symptoms such as pain, numbness, weakness, tingling, or muscle atrophy. These conditions can result from injuries, diseases, or disorders that damage or compress nerves. Common nerve conditions treated in physical therapy include:
General Treatment Methods in Physical Therapy for Nerve Conditions
Prevention of Nerve Conditions
Conclusion
Nerve conditions in physical therapy can be managed effectively with early diagnosis, proper treatment, and preventive strategies. Physical therapy plays a crucial role in reducing symptoms, improving function, and preventing the worsening of nerve-related issues. By adopting healthy lifestyle habits, maintaining good posture, and engaging in regular physical activity, individuals can reduce their risk of developing nerve conditions and improve their overall quality of life.
Spinal Conditions in Physical Therapy: Treatment and Prevention
Spinal conditions refer to disorders that affect the spine, including the bones, muscles, discs, and nerves. These conditions can cause pain, discomfort, and restricted movement, and may affect a person’s quality of life. Physical therapy plays a critical role in treating and managing spinal conditions, helping to alleviate pain, improve mobility, and prevent further damage.
Common Spinal Conditions
General Prevention and Treatment Strategies for Spinal Conditions
Conclusion
Spinal conditions can significantly impact an individual’s life, but with the right approach, many of these issues can be treated and prevented. Physical therapy plays a central role in managing spinal problems, through strengthening exercises, posture correction, manual therapy, and education on lifestyle changes. By staying active, maintaining good posture, and following proper ergonomics, most people can prevent or manage spinal conditions effectively.
What are the Cases of Paralysis in Physical Therapy, Their Treatment, and Ways to Prevent It?
Paralysis refers to the loss of muscle function in one or more parts of the body, which can occur due to a variety of reasons such as nerve injury, stroke, spinal cord injury, or neurological diseases. In physical therapy, the focus is on improving mobility, function, and overall quality of life for individuals with paralysis. It plays a crucial role in rehabilitation by offering personalized exercises, techniques, and strategies to manage and, in some cases, improve the condition.
Types of Paralysis and Their Causes
Treatment for Paralysis in Physical Therapy
The primary goal of physical therapy for patients with paralysis is to maximize function and independence by improving movement, strength, and mobility. The treatment plan will vary depending on the type, severity, and cause of the paralysis. Common physical therapy interventions include:
Prevention of Paralysis
While paralysis caused by trauma or genetic conditions may not always be preventable, there are certain steps individuals can take to reduce the risk of paralysis or improve outcomes after an injury or diagnosis:
Conclusion
Paralysis can result from various causes, including trauma, stroke, or neurological conditions, and significantly impacts a person’s life. Physical therapy plays a vital role in the treatment and rehabilitation of individuals with paralysis, focusing on improving strength, flexibility, mobility, and independence. Although not all cases of paralysis can be prevented, healthy lifestyle choices, early intervention, and injury prevention can reduce the risk of developing paralysis or help individuals achieve better recovery outcomes.
WhatsApp us