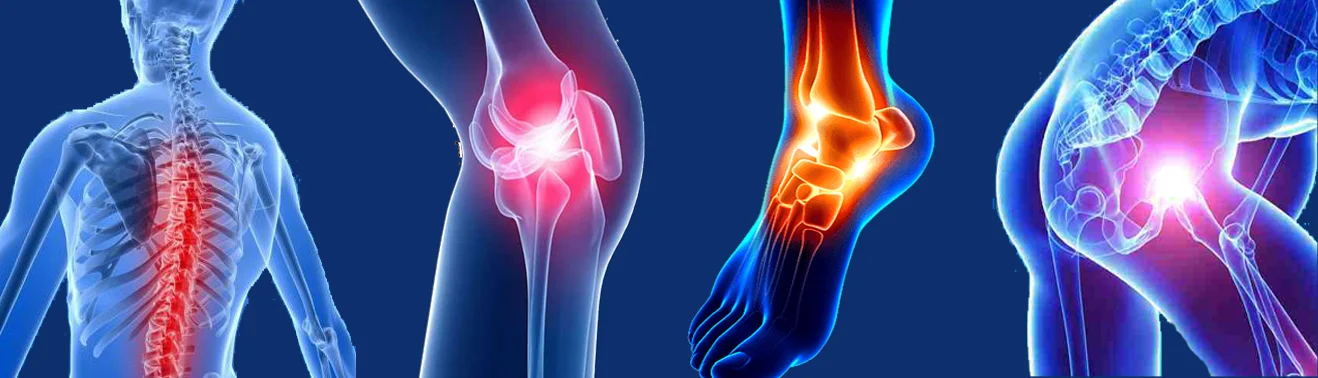
Orthopedic medicine is a medical specialty focused on the diagnosis, treatment, and prevention of musculoskeletal disorders. Orthopedic specialists, known as orthopedic surgeons, manage conditions related to bones, joints, ligaments, tendons, muscles, and nerves. They treat a wide range of issues, including fractures, arthritis, back pain, sports injuries, and congenital deformities.
Orthopedic medicine also includes non-surgical treatments such as physical therapy, medications, and injections, as well as surgical interventions like joint replacement and spinal surgery. This specialty aims to improve mobility, alleviate pain, and enhance the quality of life for patients with musculoskeletal conditions.


Orthopedic medicine includes several specialized branches, each focusing on different aspects of musculoskeletal health. These include:
These branches provide specialized care for various musculoskeletal conditions, ensuring comprehensive treatment and improved quality of life for patients.
Artificial Joint Operations (Joint Replacement Surgery) are medical procedures where a damaged or diseased joint is replaced with an artificial prosthesis or implant. These surgeries are commonly performed on joints such as the hip, knee, and shoulder, which are prone to wear and tear due to conditions like osteoarthritis, rheumatoid arthritis, or injury.
Types of Artificial Joint Operations:
Indications for Artificial Joint Surgery:
The Surgery Process:
Benefits of Artificial Joint Operations:
Risks and Complications:
Overall, artificial joint operations can provide significant relief for patients suffering from chronic joint pain and disability, helping them regain mobility and improve their quality of life.
Joint Osteoarthritis (OA) is a degenerative joint disease that primarily affects the cartilage, which is the smooth tissue that covers the ends of bones in the joint. Over time, the cartilage wears down, leading to pain, swelling, reduced flexibility, and stiffness in the affected joint. OA commonly affects weight-bearing joints such as the knees, hips, and spine, but can also affect the hands and other joints.
Causes of Osteoarthritis:
Symptoms of Osteoarthritis:
Methods of Treating Osteoarthritis:
Methods of Preventing Osteoarthritis:
Conclusion:
Osteoarthritis is a progressive condition that can affect quality of life, but with early intervention, proper treatment, and lifestyle changes, the symptoms can be managed effectively. Preventive measures like maintaining a healthy weight, regular exercise, and avoiding joint injuries can help reduce the risk of developing OA or slow its progression. For those already diagnosed, various treatments, including medications, physical therapy, and surgical options, are available to improve function and reduce pain.
Rheumatoid Arthritis (RA) is a chronic autoimmune disorder that primarily affects the joints. It occurs when the immune system mistakenly attacks the synovium (the lining of the membranes surrounding the joints), leading to inflammation, pain, and eventually joint damage. Unlike osteoarthritis, which is caused by wear and tear on the joints, rheumatoid arthritis involves an autoimmune process, meaning the body’s immune system attacks its own healthy tissues.
Causes of Rheumatoid Arthritis:
Symptoms of Rheumatoid Arthritis:
Treatment of Rheumatoid Arthritis:
There is no cure for RA, but there are several treatments that can help manage symptoms, reduce inflammation, and prevent joint damage. Treatment aims to improve quality of life and minimize the long-term effects of the disease.
Prevention of Rheumatoid Arthritis:
There is no definitive way to prevent RA, as it involves genetic and immune system factors that are not fully understood. However, there are some steps that may help reduce the risk of developing the disease or lessen the severity of symptoms:
Conclusion:
Rheumatoid arthritis is a complex autoimmune disease that can cause significant pain, swelling, and damage to the joints. While there is no cure, early treatment with medications, physical therapy, and lifestyle changes can help manage symptoms and prevent long-term joint damage. Prevention focuses on reducing known risk factors, such as avoiding smoking and maintaining a healthy lifestyle. With the right approach, individuals with RA can lead fulfilling, active lives.
WhatsApp us